
Table of Contents
Supporting Military Families With Personalized Care at Charlie Health

Written By: Elizabeth Kroll

Clinically Reviewed By: Dr. Don Gasparini
November 6, 2023
6 min.
Being part of a military family comes with unique mental health challenges. In this piece, we use data to explore how Charlie Health’s virtual Intensive Outpatient Program (IOP) effectively supports clients with military ties.
Learn more about our Clinical Review Process
Table of Contents
In the United States, there are 1.3 million active-duty service members and over 8 million veterans under the age of 65. As of 2020, approximately one-third of active military members have children, and according to the Department of Defense (DoD), there are over 1.6 million children in military families between both the active duty population and reserve service population. Having a parent in the military adds a level of stress to a child’s life that most civilians will never understand—and that can contribute to mental health challenges.
The DoD also estimates that about half of active military members are married, and the vast majority have partners who are civilians. The stress of being a military spouse comes with its own set of difficulties and emotional impacts that often benefit from mental health support.
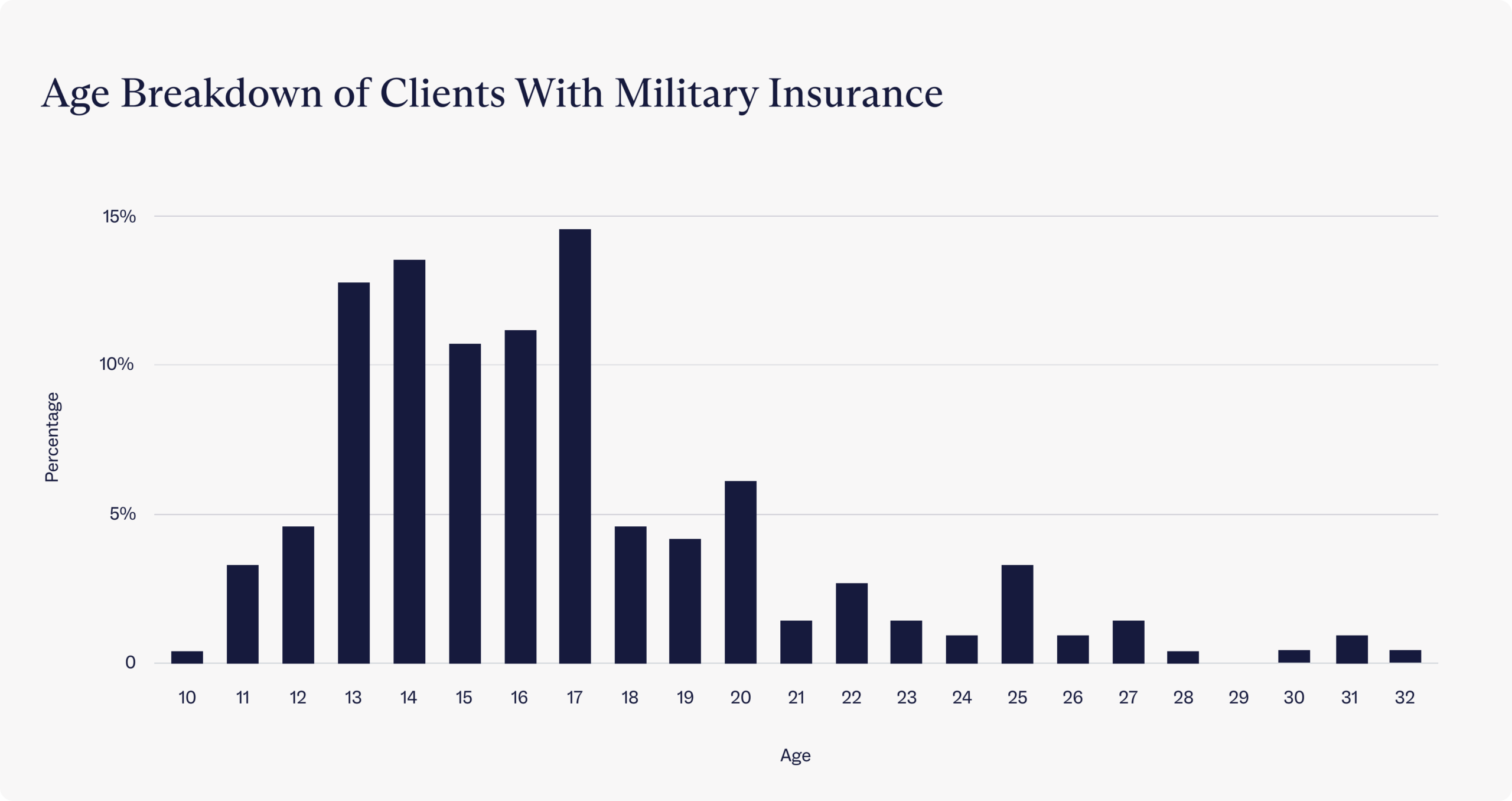
Within Charlie Health, approximately 3.6% of our clinical population lists military insurance as their primary insurance type. These clients range anywhere from 10 to 32 years old with an average age of 17. To best meet the unique needs of military families, we offer military-specific programming that helps improve clients’ outcomes—leading to decreased anxiety and depression symptoms and increased daily functioning, among other findings. Keep reading to learn more about how Charlie Health’s virtual Intensive Outpatient Program (IOP) supports the families of service members.
Mental and physical health challenges faced by military family members
Being part of a military family comes with unique mental health challenges, especially when a parent is on active duty and is deployed for any period of time. Studies show that children who have a deployed parent report significantly higher levels of psychosocial difficulties, as well as internal and external mental health symptoms such as anxiety, depression, or aggression, compared to those without a deployed parent. Approximately 22% of children with deployed parents are considered “at risk” for psychosocial morbidity both based on a parent report and a youth self-report. This is much higher than the 8 to 9% of children who are at risk and do not have a deployed parent, demonstrating just how being a part of a military family can impact a child’s mental health.

Industry-leading care for military families
Robust clinical research results in more personalized care.
Children are not the only military family members whose mental health is at risk. One study found that the highest predictor for psychosocial morbidity risk in children with deployed parents was parental stress from the parent who stayed home, emphasizing the connection between the mental health concerns of service members’ children and their spouses. An early study done with 180 spouses of deployed service members found that common emotional difficulties correlated with deployment include worry, anxiety, insomnia, and concentration problems. Additionally, army wives with deployed spouses have been found to show higher rates of depressive and anxiety symptoms. Previous research, as well as attachment theory, posits that parents who exhibit depressive symptoms from less of an emotional connection with their children, and therefore, their children are less able to process emotions and stress in a healthy way. With 42% of non-deployed parents reporting high levels of stress, it’s imperative that everyone in a military family has access to quality mental health care.
Experiencing the stress of living in a military family can also impact a person’s physical health, with members of military families showing higher heart rates, blood pressure, and BMI, plus frequent concerns with sleep, research shows. These physical symptoms can both bring on my mental health concerns and make mental illness worse. While Charlie Health programming focuses on mental health, we’ve also been able to show significant improvements in physical health over the course of treatment that may benefit military family members.
Addressing barriers to treatment for military families at Charlie Health
Data shows that military families experience multiple barriers to treatment that can make it difficult to find and maintain a therapy relationship. Here at Charlie Health, we’re addressing a few of the major barriers and improving accessibility and outcomes for military families. Here’s an overview of commonly-faced barriers to treatment for military families, and what Charlie Health is doing to make treatment more accessible to these clients:
Traveling to appointments
Military families often cite traveling to an appointment as a barrier to treatment. Families are often busy, and when service members are deployed, balancing the schedule of multiple children at a time can be stressful for the parent at home. At Charlie Health, our virtual platform allows clients to log in from anywhere confidentially, therefore reducing the travel barrier for military families. Additionally, because appointments are virtual, parents do not have to worry about finding childcare for additional children while clients are in their appointments.
Finding an appointment time
Per their busy schedules, military families often need therapy appointments in the evening or on weekends, which tend to be the hardest appointments to find. At Charlie Health, we offer groups during evening and weekend hours to make sure that clients can schedule appointments at convenient times.
Frequent moving
Military families can move frequently, with one study reporting that almost half of military family respondents moved at least three times in the past five years. According to the DoD, military families move every two to three years on average. At Charlie Health, we offer services in 27 states and counting. This means that clients are more likely to be able to remain in their program even if they have to move in the middle of treatment.
Cost
The cost of mental health treatment is a barrier across the country, especially when families have to pay out of pocket for treatment. To reduce this barrier for military families, Charlie Health partners with both Tricare East and Tricare West, as well as multiple other military insurance plans, to make sure that service members and their families have access to cost-effective mental health treatment.
Charlie Health data: military family outcomes post-treatment
As part of Charlie Health’s commitment to evidence-based quality improvement, data is collected from clients at intake and discharge. This data is used to track symptom presentation and improvement while in the program, inform quality improvement campaigns, and produce research papers. Between December 2021 and September 2023, data was collected from 235 clients who reported military insurance as their primary insurance type. Only clients who submitted intake and discharge surveys were included in this analysis. This data, across the board, demonstrates the efficacy of Charlie Health’s treatment for military families.
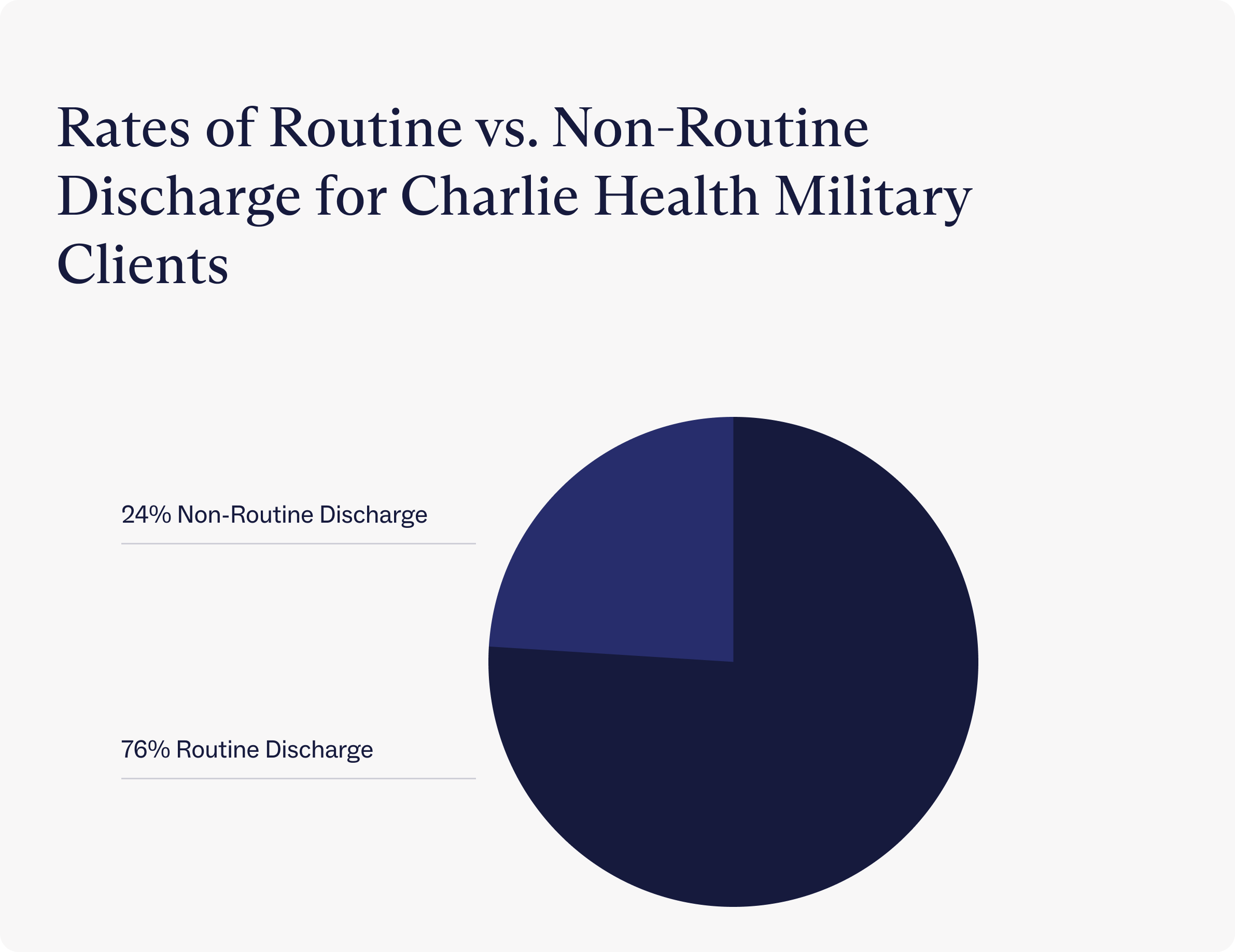
Clients with military insurance complete treatment at a 76% rate, which is higher than the industry average for IOP completion.
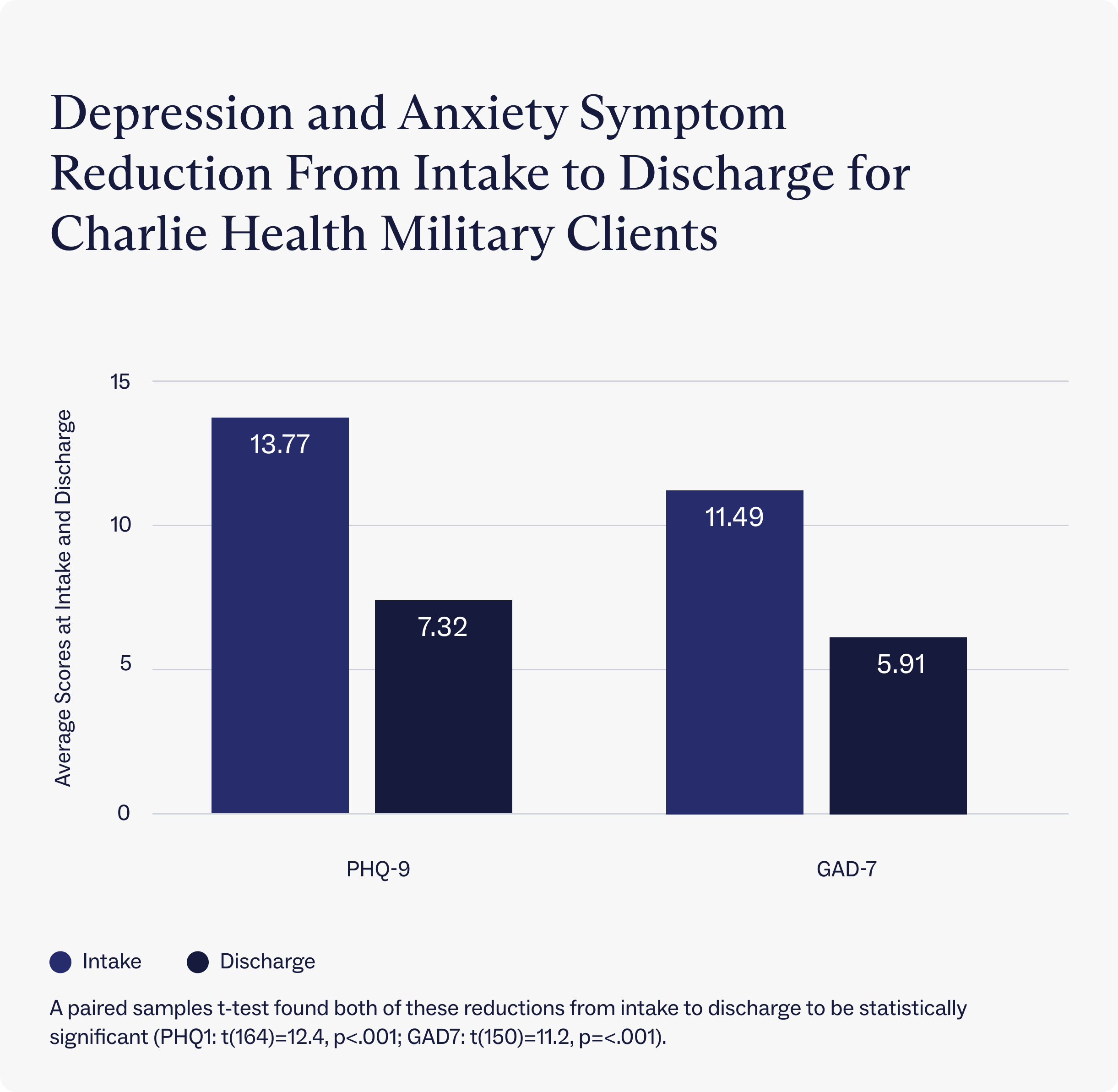
Between intake and discharge, clients with military insurance report that depressive symptoms and anxiety symptoms both decreased by 47%, as measured by the PHQ9 and GAD7, respectively. Most importantly, these reductions bring our clients below the clinical thresholds for anxiety and depression by discharge.
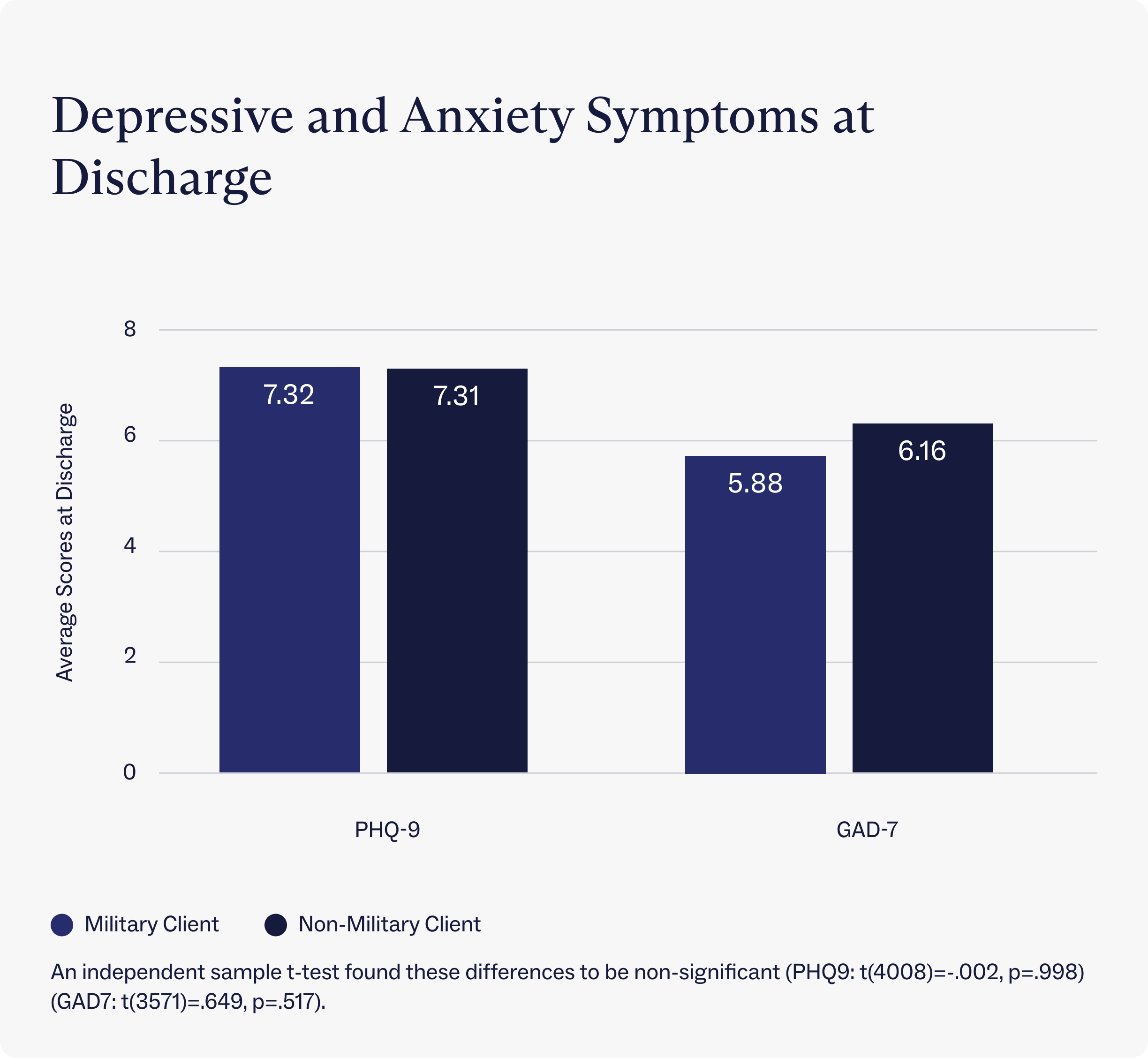
Notably, depression and anxiety scores at discharge did not vary significantly for clients with military insurance compared to the rest of our clinical population, indicating equitable improvements in symptoms between our military family clients and our civilian population. This finding is important since, as mentioned, military families often face unique barriers to treatment compared to the civilian population.
Additionally, we see a 58.24% improvement in daily functioning measured by the number of days a client’s mental health inhibits their ability to go to school or work. Before Charlie Health, clients with military insurance missed an average of nearly 3 days of work or school per-week, but after treatment they only missed an average of about 1 day of work or school per-week.
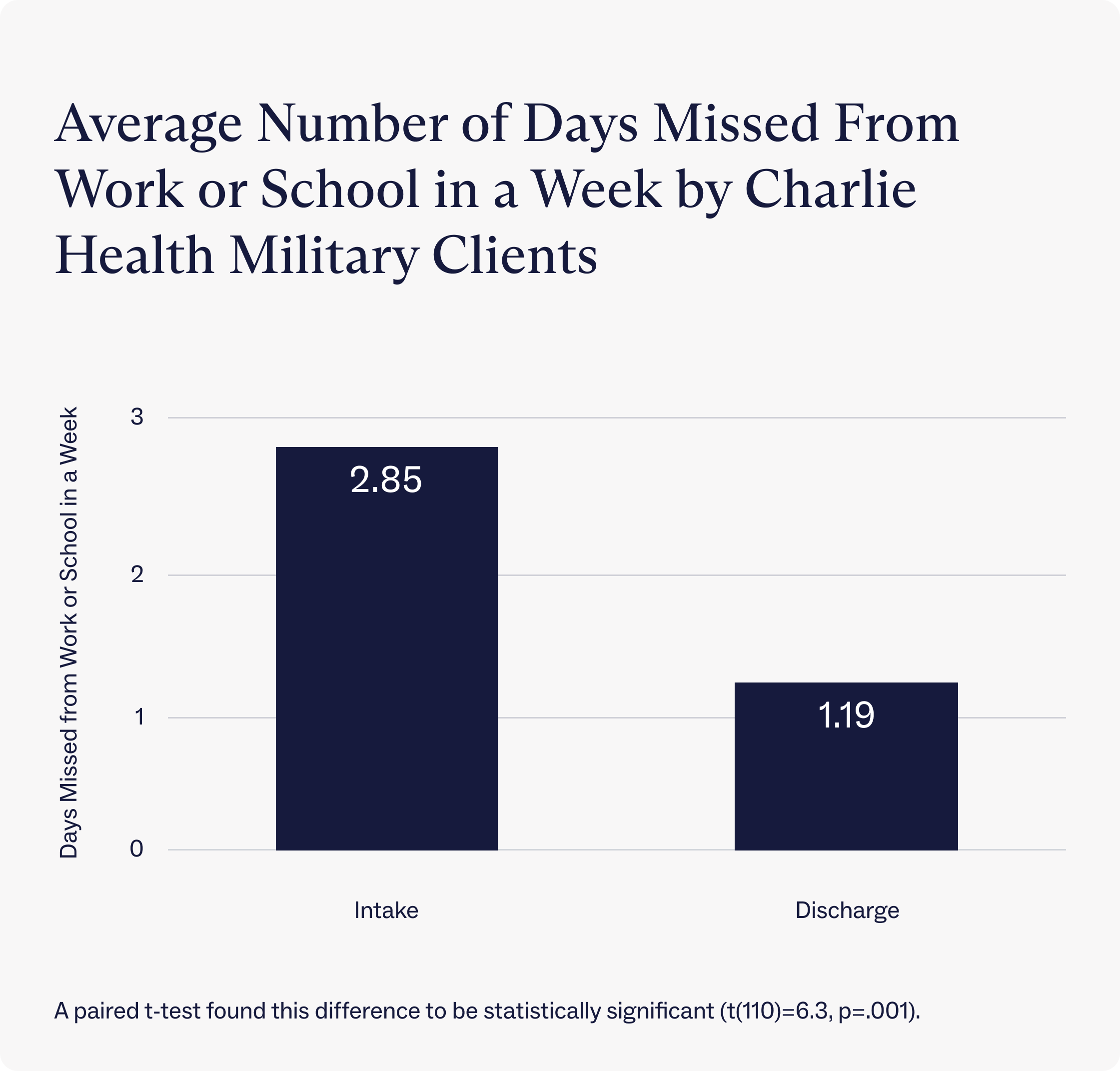
Charlie Health’s military family programming works
These findings demonstrate that with appropriate treatment, military family members can see improved mental health. Charlie Health is in a unique position to treat families of service members, and our outcomes underscore the positive impacts of our program for military families.
As an entirely virtual program with convenient scheduling, we are able to reduce the barriers to treatment that military families often face. Also, our clinicians with military cultural competency work to support military family members with their unique needs.
If you are part of a military family and need more than once-weekly mental health support, Charlie Health is here to help. Our virtual IOP combines supported groups, individual counseling, and family therapy with expert clinicians trained to work with military families. Fill out this short form to begin healing today.
References
https://download.militaryonesource.mil/12038/MOS/Reports/2020-demographics-report.pdf
https://www.charliehealth.com/post/war-trauma-psychological-consequences-of-war
https://academic.oup.com/milmed/article/176/4/402/4345324
https://psycnet.apa.org/record/1992-07414-001
https://www.charliehealth.com/post/post-traumatic-stress-disorder-treatment-for-veterans
https://www.charliehealth.com/post/secondary-trauma-and-its-impact-on-young-people
https://academic.oup.com/milmed/article/172/1/40/4578887
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4283940/
https://www.charliehealth.com/post/subtle-signs-of-depression
https://www.charliehealth.com/post/debilitating-anxiety-symptoms-causes-and-treatment
https://www.charliehealth.com/post/new-research-virtual-outpatient-care-improves-teen-mental-health




