The Library

Stay up to date on mental health research, wellness techniques, treatment services, and more
The Latest
We couldn’t find what you’re looking for.
Veteran Depression: Risks, Symptoms, and Treatment
April 3, 2026

22 Expert Tips for Maintaining a Healthy Relationship
April 1, 2026

OCD Brain vs. Normal Brain: Experts Explain the Difference
March 31, 2026

Trending

Low Dose Naltrexone: What to Avoid While Taking It, According to Experts

Clinically Reviewed By: Erin Husting

Written By: Ashley Laderer

What Is Reactive Abuse?

Clinically Reviewed By: Dr. Don Gasparini

Written By: Alex Bachert, MPH

Emotional Incest Doesn’t Mean What You Think It Means

Clinically Reviewed By: Dr. Don Gasparini

Written By: Ashley Laderer

How Common Is Sexual Assault? Look at These Statistics

Clinically Reviewed By: Dr. Don Gasparini
Written By: Charlie Health Editorial Team

7 Psychological Effects of Being Single for a Long Time

Clinically Reviewed By: Dr. Don Gasparini
Written By: Charlie Health Editorial Team

Considering Flight Anxiety Medication? Read This

Clinically Reviewed By: Courtney Way

Written By: Ashley Laderer

10 Symptoms of Daughters of Narcissistic Fathers

Clinically Reviewed By: Dr. Don Gasparini
Written By: Charlie Health Editorial Team

Anxiety Brain vs. Normal Brain, According to Therapists

Clinically Reviewed By: Cecilia Masikini

Written By: Sarah Fielding

What Stress Symptoms in Men Look Like, According to Experts

Clinically Reviewed By: Courtney Way

Written By: Sarah Fielding

The Best Ways to Lower Cortisol Levels Naturally, According to Therapists

Clinically Reviewed By: Krystal Batista

Written By: Sarah Fielding

9 Tips for How to Stop Worrying About Politics, According to Therapists

Clinically Reviewed By: Krystal Batista

Written By: Ashley Laderer

Does Anxiety Run in Families? Hear From an Expert

Clinically Reviewed By: Krystal Batista

Written By: Ashley Laderer

Political Obsession Disorder: What It Is and How to Cope

Clinically Reviewed By: Krystal Batista

Written By: Ashley Laderer

Therapist-Approved Ways to Manage Sleep Anxiety

Clinically Reviewed By: Brooke Cortez

Written By: Sarah Fielding

Therapist-Approved Ways to Manage Driving Anxiety

Clinically Reviewed By: Cecilia Masikini

Written By: Sarah Fielding

How to Overcome Flight Anxiety, According to Therapists

Clinically Reviewed By: Brooke Cortez

Written By: Sarah Fielding

Yes, Some Teens Have a Fear of Growing Up — Here’s How to Deal

Clinically Reviewed By: Dr. Don Gasparini

Written By: Britt Brewer

How to Help a Child With School-Related Anxiety, According to Therapists

Clinically Reviewed By: Austin Chason

Written By: Ashley Laderer

Therapists Explain The Link Between Cortisol and Anxiety

Clinically Reviewed By: Krystal Batista

Written By: Sarah Fielding

How to Help Someone Having a Panic Attack, According to Therapists

Clinically Reviewed By: Bree Williams

Written By: Sarah Fielding

OCD Episodes May Be Why You Feel Out of Control — Here’s How to Cope

Clinically Reviewed By: Dr. Don Gasparini

Written By: Ethan Cohen BSN, RN

Tips for Breaking the Cycle of Obsessive Thoughts and Compulsions

Clinically Reviewed By: Dr. Don Gasparini

Written By: Ethan Cohen BSN, RN

Feeling off or Disconnected? It Could Be Neurosis or Psychosis

Clinically Reviewed By: Bree Williams
Written By: Charlie Health Editorial Team

Considering Propranolol for Anxiety? Read This

Clinically Reviewed By: Bree Williams

Written By: Ashley Laderer

Your Death Anxiety Could Be Thanatophobia

Clinically Reviewed By: Brooke Cortez

Written By: Ashley Laderer

Use Our Therapist-Approved Childhood Anxiety Symptoms Checklist

Clinically Reviewed By: Nicole Lonano

Written By: Ashley Laderer

The Link Between Alcohol and Anxiety—and How to Cope

Clinically Reviewed By: Jordanne Greenberg

Written By: Ashley Laderer

The Link Between Alcohol and Panic Attacks—and How to Cope

Clinically Reviewed By: Rebecca Holland

Written By: Ashley Laderer

Here’s How Exposure Therapy for Social Anxiety Works

Clinically Reviewed By: Sarah Lyter

Written By: Sarah Fielding

Your Philosophizing Could Be Existential OCD

Clinically Reviewed By: Sarah Lyter
Written By: Charlie Health Editorial Team

Here’s What Actually Causes OCD to Get Worse—And Why

Clinically Reviewed By: Sarah Lyter

Written By: Alex Bachert, MPH

How to Help Your Teen Living With Anxiety

Clinically Reviewed By: Clary Figueroa

Written By: Sarah Fielding

Are You Worried About Vibes or Is It Emotional Contamination OCD?

Clinically Reviewed By: Dr. Don Gasparini

Written By: Ethan Cohen BSN, RN

Signs of Postpartum Anxiety That You Should Know

Clinically Reviewed By: Dr. Don Gasparini
Written By: Charlie Health Editorial Team

OCD False Memories May Be Why You Doubt the Past

Clinically Reviewed By: Dr. Don Gasparini

Written By: Ethan Cohen BSN, RN

Is It Social Anxiety Disorder or Agoraphobia?

Clinically Reviewed By: Dr. Don Gasparini
Written By: Charlie Health Editorial Team
Mental Health FAQs

Research
Stay informed with the latest insights and evidence-based strategies for enhancing your well-being
Mental Health & Relationships

5 Therapist-Approved Tips for How to Fix Attachment Issues

Clinically Reviewed By: Dr. Don Gasparini

Written By: Sarah Fielding

Here’s How to Stop Being Codependent

Clinically Reviewed By: Dr. Don Gasparini

Written By: Sarah Fielding

Yes, Being in a Toxic Relationship Affects Your Mental Health—Here’s What to Do

Clinically Reviewed By: Dr. Don Gasparini
Written By: Charlie Health Editorial Team

How to Stop Being Toxic in Your Relationships

Clinically Reviewed By: Dr. Don Gasparini

Written By: Sarah duRivage-Jacobs

Overcoming Betrayal: How to Stop Overthinking After Being Cheated On

Clinically Reviewed By: Sarah Lyter

Written By: Alex Bachert, MPH

Narcissistic Financial Abuse Signs You Should Know (and Ways to Cope)

Clinically Reviewed By: Dr. Don Gasparini

Written By: Alex Bachert, MPH

Here’s When a Sibling Rivalry Turns Into a Toxic Sibling Dynamic

Clinically Reviewed By: Dr. Don Gasparini

Written By: Ethan Cohen BSN, RN

What is Masking?

Clinically Reviewed By: Dr. Don Gasparini
Written By: Charlie Health Editorial Team

Everything You Need to Know About Dating Someone With Dismissive Avoidant Attachment

Clinically Reviewed By: Dr. Don Gasparini

Written By: Alex Bachert, MPH

22 Expert Tips for Maintaining a Healthy Relationship

Clinically Reviewed By: Brooke Cortez

Written By: Ashley Laderer

The Psychological Impacts of Family Estrangement — and How to Cope

Clinically Reviewed By: Nicole Lonano

Written By: Ashley Laderer

Battered Woman Syndrome: 12 Signs and How to Cope

Clinically Reviewed By: Courtney Way

Written By: Ashley Laderer

The Cycle of Abuse: Understanding the Stages and How to Break Free

Clinically Reviewed By: Cecilia Masikini

Written By: Ashley Laderer

Are You in Love or Is It a Trauma Bond?

Clinically Reviewed By: Dr. Don Gasparini
Written By: Charlie Health Editorial Team

Therapist-Approved Tips to Stop Self-Sabotaging in Relationships

Clinically Reviewed By: Brooke Cortez

Written By: Sarah Fielding

How to Detach From Someone

Clinically Reviewed By: Dr. Don Gasparini
Written By: Charlie Health Editorial Team

Are You in Love or Is It Limerence?

Clinically Reviewed By: Dr. Don Gasparini
Written By: Charlie Health Editorial Team

What Narcissistic Gaslighting Looks Like, According to Therapists

Clinically Reviewed By: Dr. Shanard Clemons

Written By: Sarah Fielding

A Guide to Grey Rocking in Abusive Relationships

Clinically Reviewed By: Nicole Lonano

Written By: Ashley Laderer
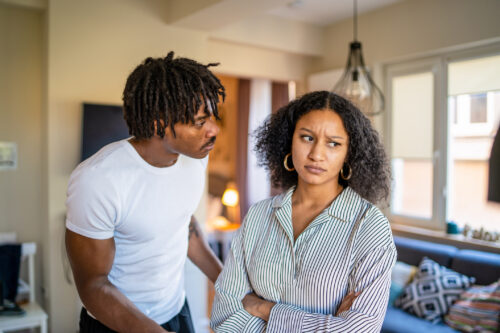
What You Should Know About Disorganized Attachment, According to Therapists

Clinically Reviewed By: Nicole Lonano

Written By: Sarah Fielding

Are Your Repeated Mistakes Actually Weaponized Incompetence?

Clinically Reviewed By: Chris Hinton

Written By: Sarah Fielding
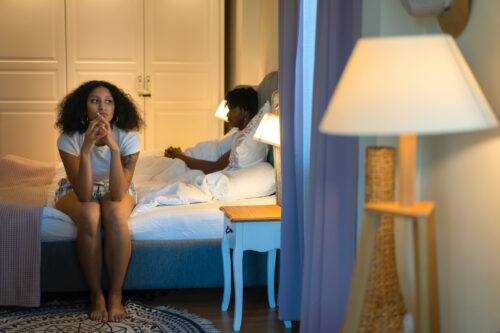
Attachment-Based Therapy Can Help You Build Healthier Relationships

Clinically Reviewed By: Courtney Way
Written By: Charlie Health Editorial Team

Future Faking Is a Relationship Abuse Tactic You Should Know

Clinically Reviewed By: Clary Figueroa
Written By: Charlie Health Editorial Team

Common Signs of An Abusive Relationship, According to Therapists

Clinically Reviewed By: Meghan Jensen

Written By: Sarah Fielding

What to Know When Dating Someone With Bipolar Disorder

Clinically Reviewed By: Sarah Lyter

Written By: Alex Bachert, MPH

How Long Does It Actually Take to Get Over Your Ex?

Clinically Reviewed By: Sarah Lyter

Written By: Ashley Laderer

Here’s What Relationship OCD Looks Like (and How to Heal)

Clinically Reviewed By: Sarah Lyter

Written By: Sarah Fielding

Overcoming Avoidant Attachment Is Possible — Here’s How

Clinically Reviewed By: Meghan Jensen
Written By: Charlie Health Editorial Team

7 Signs You’re Healing From a Breakup

Clinically Reviewed By: Meghan Jensen
Written By: Charlie Health Editorial Team

What Is Reactive Abuse?

Clinically Reviewed By: Dr. Don Gasparini

Written By: Alex Bachert, MPH

Yes, Friendship Breakups Really Hurt—Here’s How to Heal

Clinically Reviewed By: Sarah Lyter
Written By: Charlie Health Editorial Team

Is It Infatuation or Obsessive Love Disorder?

Clinically Reviewed By: Sarah Lyter
Written By: Charlie Health Editorial Team

Feeling Green With Retroactive Jealousy? Here’s How to Cope

Clinically Reviewed By: Dr. Don Gasparini
Written By: Charlie Health Editorial Team

Here’s What Conflict Avoidance Looks Like (and What to Do About It)

Clinically Reviewed By: Dr. Don Gasparini

Written By: Sarah Fielding

Is Attachment Trauma Causing Your Relationship Issues?

Clinically Reviewed By: Dr. Don Gasparini

Written By: Sarah Fielding

What Separation Anxiety in Relationships Looks Like (and How to Cope)

Clinically Reviewed By: Dr. Don Gasparini

Written By: Sarah Fielding

6 Tips to Stop Hyperfixating on a Person

Clinically Reviewed By: Dr. Don Gasparini

Written By: Dr. Rasna Kaur Neelam

What Gaslighting in a Relationship Actually Looks Like

Clinically Reviewed By: Dr. Don Gasparini

Written By: Sarah duRivage-Jacobs


Quizzes & Guides
Engage with interactive content designed to help you assess your health and navigate your journey to a healthier lifestyle
Connect with the Charlie Health community
Receive weekly updates on the latest mental health research, insights, and resources from the Charlie Health Library.
















